
Note the significant symmetric depigmentation of the face. 7 MBEH has been approved by the United States Food and Drug Administration since 1952 for permanent depigmentation of extensive vitiligo. 5, 7, 10, 11 Due to these side effects, MBEH treatment can be somewhat controversial, and its use has been limited in some countries, such as the Netherlands, which has restricted it since 1990. 5, 9 – 11 There can be repigmentation because of sun exposure or rarely as a reaction to the drug. 7, 8 Side effects of MBEH include skin irritation, contact dermatitis, ocular side effects, exogenous ochronosis, and difficulties in predicting response. 
7 Nair et al 8 have proposed that the RA enhances the absorption of monobenzone by melanocytes through the inactivation of their glutathione-dependent defense mechanisms. 7 Topical all-trans-retinoic acid (RA), a vitamin A derivative, causes mild depigmentation and when used in combination with MBEH, has synergistic effects, yielding depigmentation in a short amount of time. 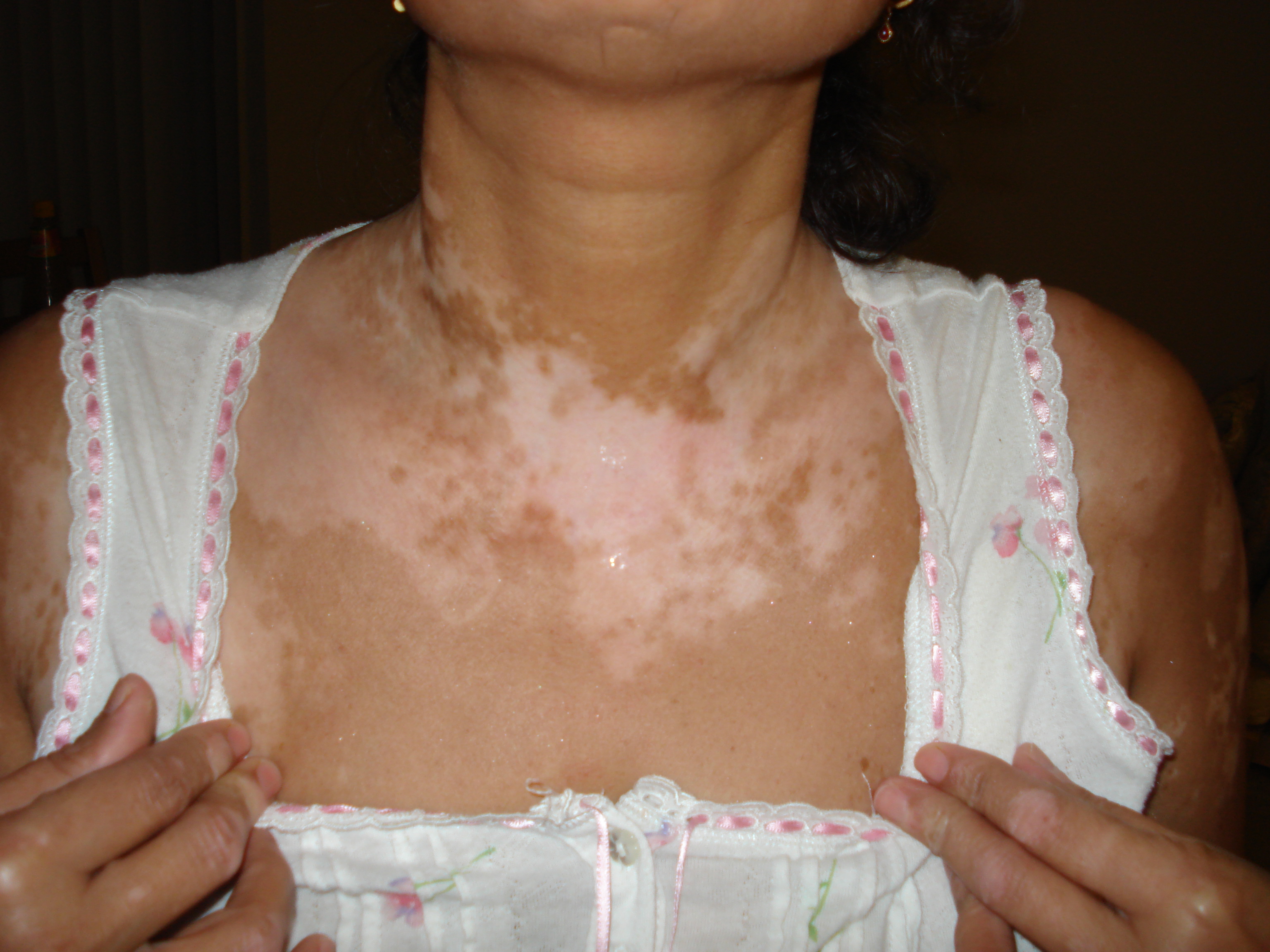
5, 7 It achieves its effects by inducing the necrotic death of melanocytes. 7 Monobenzone (monobenzyl ether of hydroquinone, MBEH) is usually the treatment of choice of depigmentation therapy for severe cases of vitiligo, and MBEH is usually used in concentrations of 20 to 40 percent to achieve the desired permanent depigmentation. Phenols, lasers, cryotherapy, and depigmenting systemic agents, such as imatinib, imiquimod, and diphencyprone, are often considered. 5 – 7 It is, however, a more aggressive approach and its use is considered on an individual basis because of the irreversible changes and increased sensitivity to sunburn of the treated areas. However, despite the type of treatment, repigmentation still remains difficult and time consuming, especially with advanced vitiligo.ĭue to the difficulties with repigmentation, it is often easier to achieve depigmentation, especially when vitiligo affects more than 50 percent of the body. 6, 7 Alternative treatments exist, such as melanocyte transplantations. 5, 6 However, PUVA can be carcinogenic and NB-UVB has low efficacy both require prolonged treatments. 6 When such treatment fails, psoralen plus ultraviolet A radiation (PUVA) and narrow-band ultraviolet B radiation (NB-UVB) are effective alternatives. 5, 6 Tactrolimus, an immunosuppressive, and calcipotriene, a vitamin D analogue, are alternative topical repigmenting agents, with a similar efficacy as the topical steroids. 6 Strong topical steroids are generally the first line of treatment, with only a 50- to 75-percent repigmentation rate. 5 Repigmentation tends to require a prolonged treatment course and yield minimal positive results. Current treatment for vitiligo attempts to either increase or decrease pigmentation in order to achieve cosmetically pleasing results and increase the patient's self-esteem. 1, 2, 4 Therefore, treatment, although not medically necessary, provides large psychosocial gains for the patient, increasing their quality of life. Studies have shown that vitiligo is associated with a greater burden of disease to patients, especially those in populations with dark skin. 1, 2, 4 Patients may feel embarrassed or ashamed of such a visible disorder. The depigmentation of vitiligo is thought to result from sexually transmitted infections, or of leprosy, and can have a damaging effect on educational, social, and employment opportunities. 
3 In some cultures, vitiligo is not well understood. The undesirable aesthetic properties of vitiligo, especially facial, may result in significant negative psychosocial effects, notably a rate of depression twice that of the general population. 2 Apart from the cosmetic appearance, it is usually asymptomatic, although there is a greater tendency for sunburns and pruritis. This is due to the acquired autoimmune destruction of melanocytes, most often in areas of greater pigmentation, such as the face and dorsum of the hands where they are most exposed to UV radiation. 2 Clinically, it appears as one or more well-circumscribed, hypopigmented, white macules or patches. 1, 2 A chronic and usually progressive disorder, vitiligo presents discretely before 20 years of age, although first presentation in later life may occur as well. Vitiligo is among one of the most common dermatological disorders, affecting up to two percent of the population worldwide.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
